- Prevalence: Alzheimer’s is much more common than LBD.
- Age of Onset: Alzheimer’s typically affects those aged 65 and older, while LBD can appear at a younger age.
Lewy Body Dementia (LBD)
LEWY BODY DEMENTIA BASICS
WHAT IS LEWY BODY DEMENTIA?
Lewy Body Dementia (LBD), also known as Dementia with Lewy Bodies (DLB), is a neurodegenerative disease that shares characteristics with both Alzheimer’s and Parkinson’s diseases. As one of the four most common types of dementia, LBD involves abnormal protein deposits in the brain, which interfere with normal brain function.
Diagnosing LBD is challenging because its symptoms often resemble those of other neurological disorders, making it difficult to identify accurately.
The Lewy Body Disease Family

Lewy Body Dementia (LBD) belongs to the Lewy Body Disease family, which includes:
- Lewy Body Dementia (LBD), also called Dementia with Lewy Bodies (DLB)
- Parkinson’s Disease (PD)
- Parkinson’s Disease with Dementia (PDD)
This guide primarily focuses on LBD, though it briefly covers PD and PDD.
Understanding Lewy Body Dementia: LBD is one of the most common causes of dementia after Alzheimer’s disease and vascular dementia. It is caused by abnormal deposits of a protein called alpha-synuclein in the brain, first discovered by Friedrich H. Lewy in the early 1900s. These deposits, known as Lewy bodies, disrupt normal brain function and cause progressive brain deterioration.
How Lewy Bodies Affect the Brain:
- Alpha-synuclein proteins are naturally present in the brain. However, in LBD, they mutate and cluster within neurons, leading to cell death.
- The location of Lewy bodies in the brain determines the symptoms:
- When they affect areas linked to motor control, symptoms may resemble Parkinson’s Disease.
- When they impact cognitive areas, symptoms may mimic Alzheimer’s Disease, affecting memory and cognition.
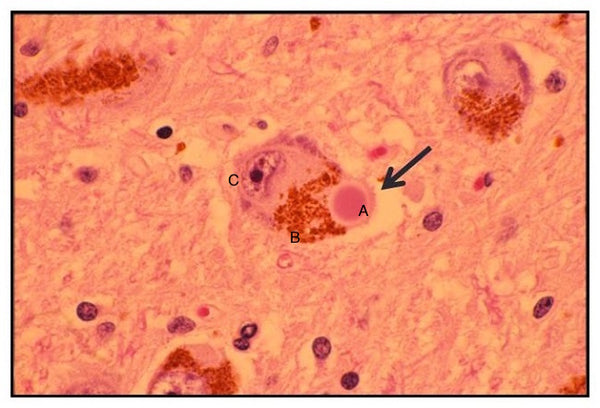
Lewy Body Pathology: H&E Stain
(A) The large pink Circle is a Lewy Body within a Brain Cell. (B) The brown section to the left of the Lewy Body is normal brain pigmentation. (C) The nucleus, the cell's control center is to the far left of the cell.
(Source: US Department of Health & Services: Advisory Council on Alzheimer's Research, Care and Services)
LEWY BODY DEMENTIA VS. ALZHEIMER'S: WHAT'S THE DIFFERENCE?
For many, Lewy Body Dementia (LBD) and Alzheimer’s disease can seem similar, and the terms are sometimes used interchangeably. However, while both are types of dementia, each has its own unique characteristics.
Key Differences
Symptom Differences
- Alzheimer’s: Usually starts with memory loss as the primary symptom.
- Lewy Body Dementia: Often begins with emotional and behavioral changes like mood swings, hallucinations, and paranoia. Symptoms may vary greatly throughout the day.

For more information on comparing the different types of dementia's - visit our Compare Diagnosis Page or visit these diagnosis specific pages:
LEWY BODY DEMENTIA VS. OTHER TYPES OF DEMENTIA
Why Diagnosing Dementia Can Be Challenging
Obtaining a clear diagnosis for dementia is difficult for physicians. Misdiagnosis or even undiagnosis is common, as no single test can definitively confirm dementia.
Diagnostic Tools
- Brain Imaging and Blood Tests: While helpful, these are not always conclusive.
- Comprehensive Cognitive Testing: Useful but not foolproof in pinpointing the type of dementia.
Despite advances in medical science, diagnosing dementia remains a complex process, as symptoms often overlap with other conditions.
Diagnosing Dementia: A Complex Process
Physicians rely on a combination of tests, the progression of symptoms, and the patient's overall deterioration to create the best possible diagnosis and treatment plan.
Types of Dementia
- Alzheimer’s Disease: 60–80% of cases
- Fronto-temporal Lobe Dementia: 5–10% of cases
- Lewy Body Dementia: 5–10% of cases
- Vascular Dementia: 10–20% of cases
Additionally, Mixed Dementia (having multiple types, such as Alzheimer’s and Fronto-temporal) is common, adding further complexity to diagnosis and treatment.
Lewy Body Dementia: Key Symptom Differences
Lewy Body Dementia primarily manifests through emotional, behavioral, and physical symptoms. Patients may experience sudden mood swings, vivid hallucinations, and motor difficulties similar to Parkinson’s.
In comparison:
- Fronto-temporal Dementia (FTD) often starts with behavioral changes like depression, compulsiveness, and apathy.
- Vascular Dementia is marked by motor function issues, such as changes in gait.
- Alzheimer’s Disease typically begins with memory loss in its early stages.
These distinctions help highlight how each dementia type uniquely affects the brain and body.
In the middle and later stages, Lewy Body Dementia (LBD) often brings about severe emotional and behavioral impairments, such as sleep disturbances, intense paranoia, hallucinations, and short-term memory loss. These symptoms are unique to LBD progression. In contrast, other types of dementia may feature increased wandering, severe memory decline, and loss of motor function. Language challenges, such as difficulty with word-finding and association, are also more prevalent in other forms of dementia.
Understanding the varied symptoms across dementia types supports accurate diagnosis and tailored treatment. Tracking these progressive changes helps physicians create individualized care plans to better manage each patient’s unique needs.
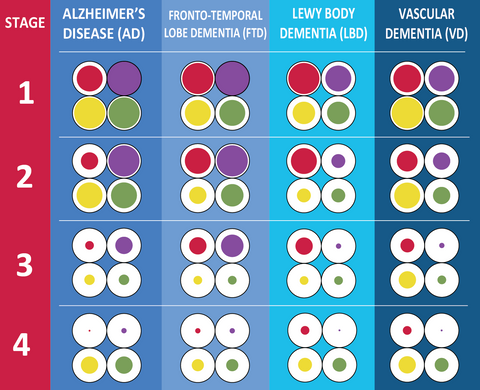
This chart provides a symptom comparison across different types of dementia, highlighting their distinct patterns.

For more information on comparing the different types of dementia's - visit our Compare Diagnosis Page or visit these diagnosis specific pages:
SYMPTOMS & STAGES OF LEWY BODY DEMENTIA
Unlike Alzheimer’s, Lewy Body Dementia (LBD) symptoms do not follow concrete stages, as the disease manifests uniquely in each individual. One person may display a distinct combination of symptoms that can fluctuate significantly—sometimes even moment to moment. These variations make LBD particularly challenging to classify into stages.
However, LBD symptoms are generally grouped into initial, core, suggestive, and supportive features. The central characteristic, shared with other dementias, is progressive cognitive decline, impacting memory, attention, and executive function over time.

The Beginning
Core Features
The main symptoms, or core features, of Lewy Body Dementia (LBD) include fluctuating cognition, hallucinations, and Parkinsonism:
- Fluctuating Cognition: This involves variations in attention and alertness, difficulty learning new skills, and impaired decision-making. To outsiders, this can sometimes seem as if the person is ‘faking’ it, though close family and friends typically recognize these changes as symptoms of the disease.
- Hallucinations: Generally well-formed and detailed, hallucinations in LBD are often most noticeable when confusion peaks. They can also involve various sensory modalities, such as sound, taste, smell, and touch. While usually not frightening, they add to the complexities of the condition.
- Parkinsonism: This includes physical symptoms such as a shuffling or stiff gait, frequent falls, and limb stiffness. Additional signs may include a ‘Parkinson’s mask’ (blank, emotionless expressions), stooped posture, drooling, and a runny nose.
These core features are distinct markers of LBD and highlight the complex, multifaceted nature of the disease.
Suggestive Features
The suggestive features of Lewy Body Dementia (LBD) are symptoms that indicate LBD once other potential causes have been ruled out:
-
REM Sleep Behavior Disorder (RBD): Often appearing years before dementia or Parkinsonism symptoms, RBD is common in LBD patients. Those with RBD may move, gesture, and even speak during REM sleep, sometimes confusing dreams with waking reality. Recent studies suggest that RBD could be a significant risk factor for developing LBD.
-
Sensitivity to Neuroleptic Drugs: Up to 50% of LBD patients experience severe sensitivity to neuroleptic or antipsychotic drugs, which can worsen symptoms such as Parkinsonism, cognitive decline, and hallucinations.
-
Low Dopamine Transporter Uptake: Low dopamine levels in the brain’s basal ganglia are also considered a suggestive feature, aligning with LBD’s characteristic symptoms.
These suggestive features provide important clues for diagnosing LBD and understanding its complexities.
Supportive Features
Supportive features are symptoms that may back up an LBD diagnosis but are not specific enough on their own, as they can appear in other neurodegenerative disorders as well. Signs in this category include:
-
Fainting Spells or Unexplained Loss of Consciousness: LBD patients may experience sudden fainting or blackouts without a clear cause.
-
Severe Autonomic Dysfunction: This involves irregularities in the autonomic nervous system, such as fluctuations in blood pressure, heart rate variability, urinary issues, constipation, and impotence.
-
Visuospatial Difficulties: LBD can impact visual processing, affecting depth perception, object orientation, and sense of direction.
-
Hallucinations in Other Sensory Modes: While visual hallucinations are common, LBD may also cause hallucinations involving sound, taste, smell, or touch.
-
Psychiatric Disturbances: Symptoms like delusions, aggression, and depression may emerge, further complicating LBD diagnosis.
These supportive features can provide additional context for diagnosing LBD and tailoring care strategies.

CAUSES, DIAGNOSIS, TREATMENTS

For more detailed information about Lewy Body Dementia including it's causes, how to detect and diagnose the disease, treatments, care options, and important resources for families caring for a loved one, check out our Lewy Body Dementia Guide at this link!
CAREGIVER TOOLS
LEWY BODY DEMENTIA CARE TIPS
Care Tips on dealing with every aspect of Lewy Body Dementia (LBD) care including how to keep your loved one safe, how to choose the right care home or tips on how to keep them at home and independent as long as possible.
Causes of LBDDetection & Diagnosis of LBDPrevention of LBDResearch of LBDSymptoms of LBDTreatments for LBD
ASSISTIVE PRODUCTS FOR LEWY BODY DEMENTIA
Find assistive products for LBD in our Lewy Body Dementia Products page. Sort by stage and symptoms to find the best products for you or your loved one.
Products by Stage:
|
Products by Symptom:
|
CARE ARRANGEMENTS

When arranging care for Lewy Body Dementia (LBD) patients, families generally choose between in-home care and out-of-home care options, based on the patient's needs and disease progression.
In-Home Care Options
For patients in the early stages of LBD, staying at home in a familiar environment can be beneficial. Initially, the primary caregiver may be able to manage care alone. However, as symptoms progress, these in-home care services can be introduced:
- Companion Services: Provide supervision, recreational activities, and companionship.
- Personal Care Services: Assist with personal tasks like bathing, dressing, eating, and exercising.
- Homemaker Services: Help with housekeeping, cooking, and shopping needs.
- Medical Care Services: Address medical needs, physical therapy, or mental health therapy as needed.
Adult Day Care Centers
For those still capable of some independence, Adult Day Care Centers offer a safe space for social interaction and recreational activities. These centers typically provide a variety of support services, such as:
- Counseling
- Health monitoring
- Meals and personal care
- Behavior management and therapy
This option helps maintain a degree of independence for the patient while giving caregivers respite.
Residential Care Options (Late Stages)
As LBD progresses, residential care becomes more appropriate to meet increased care needs. Options include:
- Personal Care Homes
- Assisted Living Facilities
- Nursing Homes with Memory Care Units
These facilities provide specialized and varying levels of care based on the individual’s needs.
Hospice and Geriatric Psychiatric Care (Short-Term)
These lesser-known short-term care options focus on supporting the patient's comfort and safety:
- Hospice Care: Available alongside any care arrangement, focusing on end-of-life comfort.
- Geriatric Psychiatric Facilities: Short-term care for adjusting medications during severe behavioral changes to ensure safety for both the patient and caregivers.
For additional guidance on care arrangements or to explore detailed comparisons of each option, visit our pages on:
- Care at Home
- Adult Day Care
- Assisted Living
- Nursing Home
SUPPORT & RESOURCES
- Lewy Body Dementia Association: Support Group Listing
- Online Forums & Chat Rooms:
- Lewy Body Dementia Association Forum: Lewy Body Dementia Association Forum
- Alzheimer's Association: AlzConnected
- Facebook Groups:
- Anonymous chat rooms for Free therapy: 7 Cups
For family members and friends who would like to educate themselves further on the details of Lewy Body Dementia, its symptoms, treatments, and challenges, you should seek the assistance of the national Lewy Body Dementia Association as well as other organizations listed below:
Other websites to obtain more detailed information on Lewy Body Dementia:
LEWY BODY DEMENTIA RESEARCH
FINDING A PHYSICIAN
Generally, the majority of doctors who recognize and diagnose Lewy body dementia are neurologists–and specifically neurologists who specialize in dementia and movement disorders.
For a list of providers, follow this link.
CLINICAL TRIALS
Compared to Alzheimer’s, LBD is still a relatively unknown type of dementia. And because of that, there are a lot of ongoing research and clinical trials going on every day. For example, there are:
- Treatment trials where new and existing drugs are tested to study it has a positive effect on the symptoms of LBD.
- Genetics studies where scientists try to figure out whether LBD is a genetically passed down disease.
- Diagnostic studies where scientists and researchers look for better and improved alternative ways of diagnosing the onset of LBD.
- Prevention trials where researchers investigate ways of preventing the onset of LBD itself.
For more information on research currently being conducted on Lewy Body Dementia, the following are great resources and tools that can help shine light on progress being made.
- Lewy Body Dementia Association: Research
For a list of clinical trials check out these awesome resources:
- ClinicalTrials.gov: Provides regularly updated information about federally and privately supported clinical research in human volunteers. ClinicalTrials.gov gives you information about a trial's purpose, who may participate, locations and phone numbers for more details.
- NIH Clinical Research Trials and You: Is an online resource to help people learn more about clinical trials, why they matter and how to participate. Provides information on the basics of clinical trial participation, first hand experiences from actual clinical trial volunteers, explanations from researchers, and links on how to search for a trial or enroll in a research matching program.
- Fox Trial Finder: Is a web-based clinical trial matching tool to connect those with and without Parkinson's disease to Parkinson's clinical research participation opportunities. Also provides the opportunity for volunteers to connect directly with trial coordinators through a secure messaging interface on the site.
- Alzheimer's Association: Lists selected trials in treatment and prevention of Alzheimer's disease from ClinicalTrials.gov. Trials included here are recruiting participants at more than one U.S. location.
- Center Watch: Clinical research, including listings of more than 41,000 active industry and government-sponsored clinical trials, as well as new drug therapies in research and those recently approved by the FDA.
Disclaimer
All text, charts, graphics, images, videos, downloads, and tools on this page (“Content”) are for general educational purposes only and are not medical advice. Dementia varies by person and diagnosis is complex; summaries and comparisons are simplified. We do not guarantee accuracy or completeness. Use at your own risk. To the fullest extent permitted by law, Dementia Aide LLC disclaims liability for any loss or damages arising from use of or reliance on the Content.
Copyright: © 2026 Dementia Aide LLC. All rights reserved.