Vascular Dementia (VD)
VASCULAR DEMENTIA BASICS
WHAT IS VASCULAR DEMENTIA?
Vascular dementia is the subtle progressive worsening of memory and other cognitive functions that can be attributed to vascular disease within the brain. In people with this condition, symptoms of dementia, such as memory loss and difficulty with thinking, language, and problem solving, occur due to brain damage caused by blood supply problems in the brain. The problems could be a block or lack of blood flow to the brain. Reduced blood flow in turn, deprives the brain of oxygen. Together, it can cause brain damage, even in a short period of time.
Also known as vascular cognitive impairment, the condition accounts for an estimated 10% of dementia cases, although, many experts believe that it is underdiagnosed. As with dementia in general, people above the age of 65 are at a higher risk of being diagnosed.
Vascular dementia is caused by reduced blood flow to the brain, which damages and eventually kills brain cells. This can happen due to a number of reasons such as the narrowing of small blood vessels deep inside the brain, aneurism, a stroke, or several mini-strokes. Sometimes, the damage could also be due to Alzheimer’s. In such cases, it is known as mixed dementia.
 |
 |
Multi-infarct Dementia
Binswanger’s Disease
VASCULAR DEMENTIA VS. ALZHEIMER'S
To the average person, Vascular Dementia and Alzheimer's often seem like the same thing. Sometimes, the two terms are even used interchangeably. However, although the two are somewhat related, each condition has its own distinct differences.
Both Vascular Dementia and Alzheimer's are types of dementia. Alzheimer's is much more common then VD and symptoms of the diseases vary significantly. While Alzheimer's typically affects in the late stages of life (65+), Vascular Dementia can start to show symptoms at an earlier age and are typically prompted abruptly by a stroke in the brian.
Typically, the first symptoms of Alzheimer's are memory loss, whereas early Vascular Dementia symptoms are primarily loss of motor function, slurred speech, and impairment in executive function.
To compare types of dementia's - visit our Compare Diagnosis Page or visit these diagnosis specific pages:
VASCULAR DEMENTIA VS. OTHER TYPES OF DEMENTIA
Obtaining a clear diagnosis for dementia is extremely difficult for physicians.
Misdiagnosis and undiagnosed is common in dementia because while brain imaging, blood testing, and comprehensive tests can help in the diagnosis, it is still not a perfect science. Physicians rely on the tests as well as the progressing deterioration and occurrence of different symptoms to make as best of a diagnosis and treatment plan as possible.
While there are many types of dementia, the four largest subset of dementias are Alzheimer's (estimated at 60%-80% of the cases), Fronto-temporal Lobe Dementia (estimated at 5-10% of cases), Lewy Body Dementia (estimated at 5-10% of cases), and Vascular Dementia (estimated at 10-20% of cases). Mixed dementia - or having multiple types of dementia (example: Alzheimers and Fronto-temporal Lobe) is also common in dementia patients, making it even more complex to diagnose and treat.
Vascular Dementia specifically compared to other symptoms shows itself primarily with slowness in thought, changes to the persons gait, and trouble with language. Memory loss is most prevalent in the early stages of Alzheimer's and in Lewy Body Dementia, drastic fluctuations in mood or behaviors, vivid hallucinations and motor difficulties similar to parkinsonism. By comparison, behavioral issues such as depression, compulsiveness and apathy are more prominent in the earlier stages of Fronto-temporal Dementia (FTD).
Towards the middle and later stages, patients with Vascular Dementia show pronounced loss of physical capabilities such as urinary disturbances, speech difficulties and slowness in thought. In contrast, Alzheimer's and FTD patients tend to suffer from wandering, progressed memory loss, and issues with word finding and word association. Patients with LBD show progressed behavioral and emotional disturbances such as sleep disorders, vivid hallucinations and severe paranoia.
Being informed about the other types of dementias and symptoms experienced by those who have it, assists in the diagnosing and treating of the disease. It is extremely important to take note of the progressive changes of symptoms as this will enable the physician to make customized treatment and medication plans to counter the symptoms of the disease.
This chart compares the symptoms of the different types of diseases to show what types of symptoms are more or less in the various diseases.

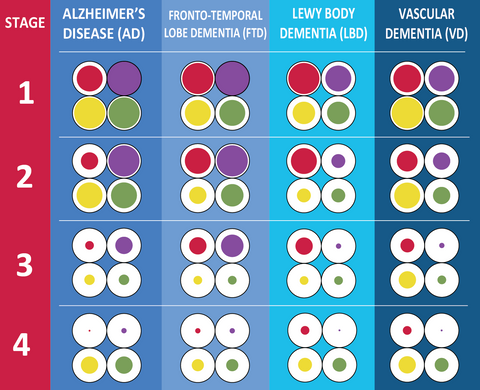
For more information on comparing the different types of dementia's - visit our Compare Diagnosis Page or visit these diagnosis specific pages:
SYMPTOMS & STAGES OF VASCULAR DEMENTIA
Symptoms of Vascular Dementia can often overlap with symptoms of Alzheimer’s, but is largely dependent on the location of impaired blood flow within the brain. It is easiest to identify the symptoms when it occurs after a stroke. In cases where the patient suffers multiple strokes or mini strokes, the progression of the symptoms tend to be more stepwise, abrupt and noticeable rather than the steady decline you find in other cases of dementia. As is the case with all types of dementia, the progress of vascular dementia on each individual is different. However, it only worsens over time. The many signs of vascular dementia can be divided into three categories: mental & emotional, physical, and behavioral.
Stage 1: Behavioral Deterioration
Stage 2: Early Stages
Stage 3: Middle Stages
Stage 4: Late Stages
This infographic summarizes symptoms experienced at general progressions of Vascular Dementia. Symptoms in bold are more common in VD than in other types of dementia:

CAUSES, DIAGNOSIS, TREATMENTS

For more detailed information about Vascular Dementia including it's causes, how to detect and diagnose the disease, treatments, care options, and important resources for families caring for a loved one, check out our Vascular Dementia Guide at this link!
CAREGIVER TOOLS
VASCULAR DEMENTIA CARE TIPS
Care Tips on dealing with every aspect of Vascular Dementia (VD) care including how to keep your loved one safe, how to choose the right care home or tips on how to keep them at home and independent as long as possible.
CARE ARRANGEMENTS

In terms of care arrangements for VaD patients, there are generally two types of options that the patient’s friends and family can opt for: in-home care or out-home care.
During the initial stages, while the patient is still able to function independently, most people may prefer to remain at home, where they are most familiar with their surroundings.
After initial diagnosis, the primary caregiver may still be able to handle the tasks of looking after the patient. But as the symptoms progress to the early and middle stages, they can opt for in-home care arrangements. There are several types available in this category:
- Companion services – to help with supervision and recreational activities.
- Personal carers – to help with various personal care tasks such as bathing, dressing, eating, and exercising.
- Homemaker services – to help with housekeeping, cooking, or shopping.
- Medical carers – to help with medical needs, physical, and/or mental therapies
Another option for patients who are still able to function relatively independently, is Adult Day Care Centers. These facilities provide a safe environment for dementia patients to pursue activities, interests, and socially interact with people. This type of care arrangement can give the patients a sense of freedom while dealing with their diagnosis. They are also likely to have counselling, health services, meal services, personal care, behavior management, therapy, and other related services available.
During the last stages of dementia, when the patient is unable to fend for themselves, the best choice often will be residential care in the form of Personal Care Homes, Assisted Living, Nursing Homes with special care or memory units. There, they can receive specialized care and treatment to ease their situation. Each of these facilities will offer different levels of care. Selecting one will depend on the patient’s needs and progression of Vascular Dementia. Read our detailed guides on each one to assess which may be the best fit for you or your loved one.
Hospice Care and Geriatric Psychiatric Facilities are two lesser talked about short-term arrangements for patients with dementia. These systems assist with end of life comfort measures (hospice) and medication rebalancing (Geriatric Psychiatric Unit), both of which are crucial to maintaining the patient’s dignity and safety for them and their caregivers.
Hospice Care services are available with any care arrangement and are attached to the patient wherever they go as long as the organization providing the services is able to provide services.
Geriatric Psychiatric Facilities are meant to be a resource for when a patient is experiencing severe behavioral changes that need to be adjusted for with medication in order to ensure the patients, and his/her caregivers safety.
For more information on the differences, how to find a care facility and on commonly experienced issues with each care arrangement, visit the following pages:
- Care at Home
- Adult Day Care
- Assisted Living
- Nursing Home
SUPPORT & RESOURCES
Other websites to obtain more information on vascular dementia:
VASCULAR DEMENTIA RESEARCH
FINDING A PHYSICIAN
For a list of providers close to your area, follow this link.
CLINICAL TRIALS
As is the case in almost any facet of the medical field, there is constant research and development being done with regards to vascular dementia. The following is a list of types of clinical trials that are being done:
- Treatment trials—to find more effective blood thinners, anticoagulants, and any drug that can reduce the risk of blood clots and strokes.
- Diagnostic studies—to find new tests and methods to diagnose vascular dementia earlier and more accurately.
- Prevention trials—to explore various means of preventing the formation of blood clots and resulting strokes.
- Quality of life studies—to explore ways to improve the quality of life for patients and caregivers at different stages of the illness’s progression.
Disclaimer
All text, charts, graphics, images, videos, downloads, and tools on this page (“Content”) are for general educational purposes only and are not medical advice. Dementia varies by person and diagnosis is complex; summaries and comparisons are simplified. We do not guarantee accuracy or completeness. Use at your own risk. To the fullest extent permitted by law, Dementia Aide LLC disclaims liability for any loss or damages arising from use of or reliance on the Content.
Copyright: © 2026 Dementia Aide LLC. All rights reserved.
